First-in-human trial demonstrates safety of sonobiopsy in patients with glioma
Getting a biopsy is often an important first step for cancer diagnosis and treatment. But brain tumors present unique challenges: to perform a biopsy, a neurosurgeon will likely need to drill into the skull, and removing brain tissue can cause complications, including bleeding, brain swelling, or infection. Promising methods to noninvasively diagnose brain tumors have remained elusive—until now.
A collaborative team of NIH-funded researchers is developing a way to obtain DNA shed from brain tumors using focused ultrasound. Their first-in-human study, reported in the Nature journal npj Precision Oncology, could be an important step towards improving the way brain tumors are diagnosed.
“Focused ultrasound is conventionally used as a therapeutic technique, where high-intensity ultrasound waves are directed at a single focal point to destroy problematic tissue,” explained Randy King, Ph.D., a program director in the Division of Applied Science & Technology at NIBIB. “The method described here turns that paradigm on its head, harnessing focused ultrasound not for treatment, but for a diagnostic purpose.”
Sonobiopsy: focused ultrasound meets liquid biopsy
Traditional biopsy approaches involve cutting into the body to remove a sample of suspicious or cancerous tissue, which is then analyzed to direct treatment approaches. Tumors, nonetheless, can shed bits of their DNA into the bloodstream, which can also be collected and analyzed. This approach, known as a liquid biopsy, is used clinically for some types of cancer and has several advantages, such as the ability to noninvasively sample tumor DNA many times over.
However, it’s very challenging to capture DNA shed from tumors in the brain. The brain is surrounded by a protective vascular network known as the blood-brain barrier, which stops certain substances from passing through. This barrier works in both directions: potentially harmful molecules can’t easily enter, and materials in the brain can’t easily leave, either.
Enter sonobiopsy. This technique uses focused ultrasound to mechanically disrupt the blood-brain barrier, allowing small molecules (like tumor DNA) to pass through. Once in the bloodstream, the tumor DNA can be collected using a simple blood draw and analyzed to gather information about a patient’s cancer.
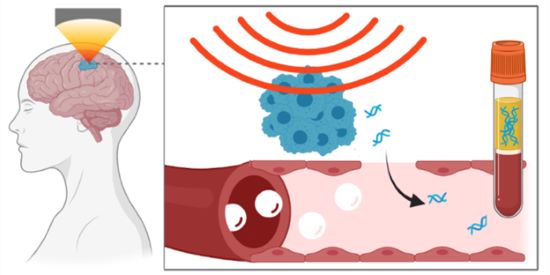
“The concept of using focused ultrasound to temporarily open the blood-brain barrier is not new—in fact, it has been under development for more than two decades,” explained co-senior study author Hong Chen, Ph.D., associate professor at Washington University in St. Louis. “But these efforts have largely focused on opening the blood-brain barrier to allow drugs in the bloodstream into the brain to treat brain diseases. Our team is trying to get molecules out of the brain—specifically, DNA shed from brain tumors.”
Opening the blood-brain barrier using focused ultrasound relies on the presence of microbubbles. These microbubbles are FDA-approved contrast agents that are traditionally used to enhance ultrasound imaging techniques. They can circulate in the blood vessels throughout the body, including those around the brain. When the microbubbles are exposed to acoustic pressure—such as focused ultrasound waves—they expand and contract. The repeated expansion and contraction of the microbubbles subsequently pushes and pulls on the vessel walls. This mechanical force puts stress on the blood-brain barrier, enhancing the permeability of the blood vessels and ultimately allowing small molecules to pass into or out of the brain.
Evaluating sonobiopsy in a first-in-human clinical trial
In this study, the researchers introduced a compact focused ultrasound device that can be seamlessly integrated into existing clinical workflow. Their first-in-human clinical trial, led by co-senior study author Eric Leuthardt, M.D., Shi Hui Huang Professor of Neurosurgery at Washington University School of Medicine, evaluated the sonobiopsy device in five patients with high-grade gliomas, an aggressive type of tumor that develops in the brain. Each of these patients were scheduled to undergo brain surgery to remove their tumors. Immediately before the surgery, the researchers performed a sonobiopsy by steering focused ultrasound waves directly at the brain tumor. Blood samples were collected before and after the procedure, and then the patients had their tumors removed. Both the blood samples and the removed tumor tissue were analyzed after the surgery.
Using the tumor tissue removed from the brain, the researchers were able to identify tumor-specific DNA sequences for each patient. They used this information to determine if the DNA found in the bloodstream following the sonobiopsy procedure originated from the tumor in the patient’s brain. Their analyses revealed that sonobiopsy significantly enhanced the detection of tumor-specific DNA in the bloodstream in three of the five patients. Notably, for one patient, the amount of tumor DNA detected in the bloodstream nearly doubled.
“We are still in the developmental stage of this technology, and our trial was designed to use the tumor tissue taken from the brain as a benchmark to determine if the DNA found in the bloodstream was shed from the tumor following the sonobiopsy procedure,” explained Leuthardt. “After we fully validate our method, the ultimate goal is to use a sonobiopsy to noninvasively analyze lesions in the brain to understand their molecular and genetic makeup to guide treatment decisions.”
Even though the sonobiopsy did not increase tumor-specific DNA in the bloodstream among all five patients, Chen noted this finding was expected. “Because this is a first-in-human trial, the ultrasound parameters that we used were likely not optimal,” she said. “We erred on the side of caution to make sure that the ultrasound parameters were as safe as possible for our patients. Given this approach, the fact that the procedure resulted in increased circulating tumor DNA for more than half of our patients was very encouraging.”
In terms of safety, the researchers did not observe any detectable tissue damage on the surface of the brain following the sonobiopsy procedure, and microscopic analysis of the removed tumor tissue did not reveal any apparent injury to regions that were exposed to focused ultrasound.
“In addition to demonstrating the feasibility of our approach, this first-in-human prospective trial suggests that sonobiopsy has the potential to transform the precision diagnosis of brain tumors and other neurological disorders,” said Chen. “While our early data is promising, further studies with larger sample sizes are needed to confirm these initial findings and establish the clinical utility of sonobiopsy.”
Study reference: Yuan, Jinyun et al. “First-in-human prospective trial of sonobiopsy in high-grade glioma patients using neuronavigation-guided focused ultrasound.” NPJ precision oncology vol. 7,1 92. 16 Sep. 2023, doi:10.1038/s41698-023-00448-y
This study was supported by grants from NIBIB (R01EB027223 and R01EB030102), the National Cancer Institute (NCI; R01CA276174), the National Institute of Mental Health (NIMH; R01MH116981 and UG3MH126861) and the National Institute of Neurological Disorders and Stroke (NINDS; R01NS128461).
