- What are sensors and how are they used?
- How are sensors used in biomedical research and medical care?
- What are NIBIB-funded researchers developing in the area of sensors to improve biomedical research and medical care?
What are sensors and how are they used?
Sensors are tools that detect and respond to some type of input from the physical environment.
There are a broad range of sensors used in everyday life, which are classified based on the quantities and qualities they detect.
Examples include electric current, magnetic or radio sensors, humidity sensors, fluid velocity or flow sensors, pressure sensors, thermal or temperature sensors, optical sensors, position sensors, environmental sensors, and chemical sensors.
How are sensors used in biomedical research and medical care?

In medicine and biomedical research, there are many types of sensors that are used to detect specific biological, chemical, or physical processes that then transmit or report this data to individual users or healthcare professionals.
- Thermometers translate the expansion of a fluid or bending of a metal strip in response to heat into a value that corresponds to body temperature.
- Wearable technologies such as smartwatches carry sensors that can track, analyze, and transmit data about heart rate and sleep patterns. Researchers are using wearables to monitor the health of individuals and even predict and potentially intervene to prevent acute health events such as stroke or heart attack.
- Pulse oximeters measure changes in the body’s absorption of special types of light to measure heart rate and the amount of oxygen in the blood. These sensors are frequently used in hospitals and clinics and can also be purchased for at-home use.
While many advanced sensors aren’t practical for routine medical care, they allow researchers to study and learn about the basic foundations of disease, potentially facilitating the development of new technologies.
What are NIBIB-funded researchers developing in the area of sensors to improve biomedical research and medical care?
Circulating nanosensors for continuous drug monitoring. NIBIB-funded scientists are developing sensors that circulate in the blood and continuously monitor drug concentrations to help maintain therapeutic levels and avoid high, toxic levels. The sensors send a fluorescent signal that changes with drug concentration and can be detected through the skin. To allow the sensor to remain in the blood without being eliminated from the body, the sensors are “hidden” in red blood cell (RBC) “ghosts,” which are the outer shell of the RBC. In experiments in mice, sensors designed to detect lithium carried inside the RBC ghosts remained in the blood stream for weeks sending a fluorescent signal that accurately measured the lithium levels in the blood. The circulating nanosensors could improve drug effectiveness by allowing physicians to monitor and adjust drug concentrations to maintain optimal therapeutic levels.
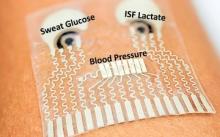
Smart textiles for prevention of deep vein thrombosis. Deep vein thrombosis (DVT) is the formation of blood clots in the legs. Caused by limited mobility in hospital patients, the elderly, and pregnant women, DVT can result in pulmonary embolism (PE), a life-threatening condition that occurs when clots from the legs travel to the lungs and become lodged in the pulmonary arteries. NIBIB-funded researchers are using smart textiles to prevent DVT and reduce the occurrence of PE. The smart textiles carry sensors that do not require batteries and are woven directly into socks and other garments. The smart textiles can remotely detect movement or lack of movement that would promote DVT and automatically provide mechanical stimulation to block the formation of blood clots. The approach aims to dramatically reduce the more than 200,000 cases of PE that occur in the U.S. each year.
Inexpensive genetic sensor for zinc deficiency. In developing countries, lack of the micronutrient zinc in mothers’ diets is associated with fetal growth retardation, impairment of learning and memory function, and increased morbidity and mortality in children. To enable widespread testing for zinc deficiency, NIBIB-funded scientists are using synthetic biology to create an inexpensive zinc sensor for use in low-resource settings. The approach involves engineering bacteria that give a color read-out in response to the amount of zinc in a blood sample. Different colored read-outs are based on the zinc concentration in the sample, indicating whether zinc levels are acceptable or too low (which would indicate the need for zinc supplements). The portable, minimal-equipment bacterial biosensor for blood micronutrients would enable large-scale studies on nutritional interventions to better treat millions of undernourished people in low-resource settings.
Updated April 2022
