Custom printed models could improve fit and function of replacement valves
Every year thousands of Americans, mostly over age 75, require replacement of their aortic valve. Now 3D printed patient-specific models of the aorta can aid presurgical planning and improve outcomes of minimally invasive valve replacement.
The left ventricle of the heart has the important function of pushing fresh oxygenated blood through to the aorta, which then distributes blood throughout the body. The aortic valve opens as the blood is pushed through and then closes so blood cannot move backwards into the heart. Aortic stenosis is a condition where the aortic valve has become narrow over time, causing the heart to work harder—a condition that can lead to heart failure.
Transcatheter aortic valve replacement (TAVR) is a procedure where an artificial heart valve is threaded with a catheter through the aorta and expanded—much like opening an umbrella—to replace a failing aortic valve. TAVR is increasingly being used because it is a minimally invasive procedure that is much safer than open heart surgery for the predominantly elderly patients who require the procedure. However, because of irregularities of the diseased valve and patient-specific contours of the aorta, getting a perfect leak-proof fit and optimal positioning of the new valve is not always assured.
Now NIBIB-funded engineers at the University of Minnesota, led by Michael McAlpine, who holds the Kuhrmeyer Family Chair Professorship in the University of Minnesota Department of Mechanical Engineering, have made significant inroads toward improving TAVR by 3D printing a precise model of a patient’s diseased valve and surrounding parts of the aorta. This physical model of the region—known as the aortic root—allows physicians to practice the procedure needed for each patient, allowing them to identify the right size replacement valve and determine the exact placement in the aorta that will give the best fit and function.

“As the US population ages, the number of individuals over 75 needing valve replacement using TAVR will continue to grow,” explained Michael Wolfson, director of the NIBIB program in bionic systems. “The ability to create patient-specific models of the aortic root is a major development that could improve the success rate of this challenging procedure and significantly reduce the risks of postoperative complications.”
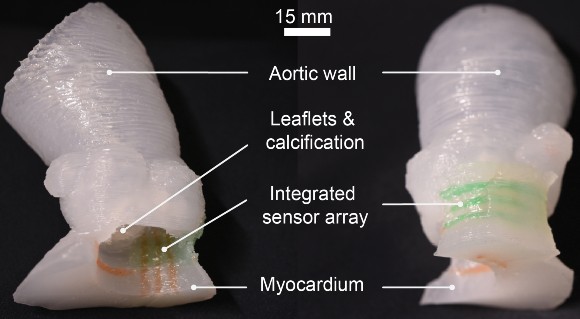
Although aortic root models have been used before for surgical planning, the models created by the advanced 3D printing technique are much more lifelike in texture and elasticity. Another unique aspect of these models is the incorporation of sensors in the wall of the aorta. The sensors provide feedback that allows physicians to avoid the application of excessive pressure by the replacement valve to the conduction pathway that controls heart rhythm. Too much pressure can cause abnormal heart rhythms and the immediate need to implant a permanent pacemaker in the patient.
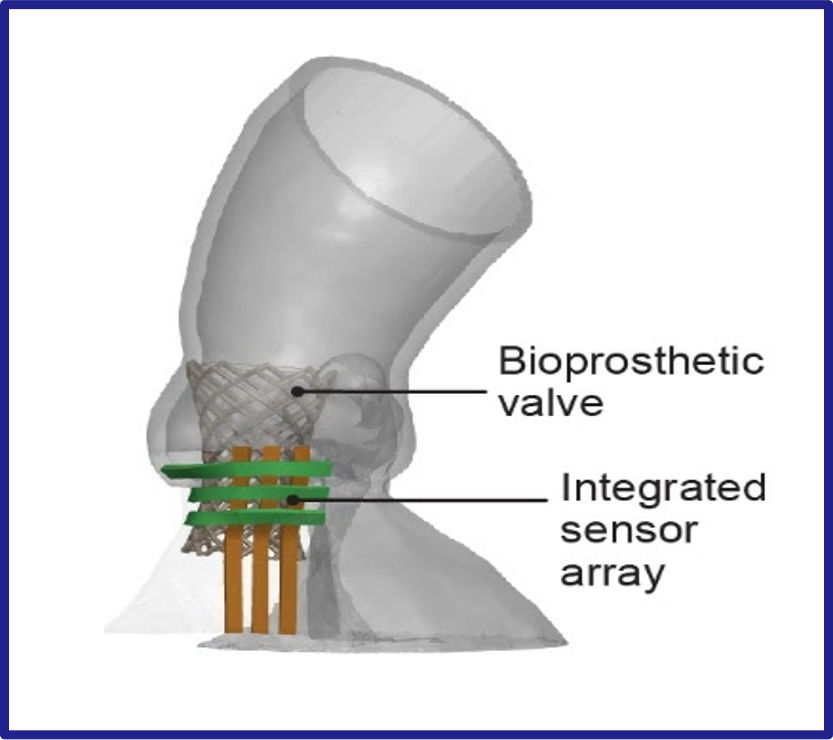
The engineering team uses CT scans of the patient’s heart to recreate the exact shape of the aortic root region. They are then 3D printed with specialized silicone-based inks that match the feel of real heart tissue. The soft electric sensors that give pressure feedback are also 3D printed into the model and are made of a conducting hydrogel.
"This 3D-printing process was designed to help physicians improve the outcomes of the TAVR procedure and can also help give patients a clearer understanding of their anatomy and how the procedure works” said McAlpine. As engineers continue to improve 3D printing techniques and create even more lifelike models of organs, McAlpine envisions where such technologies could lead. “In the future, as our 3D-printed models incorporate more aspects of organ function, we see the potential for the models themselves to someday be used as artificial replacement organs."
The work was reported in the journal Science Advances1. Funding was provided via grants from the National Institute of Biomedical Imaging and Bioengineering (DP2EB020537), Medtronic plc, and the MnDRIVE program at the University of Minnesota.
