Preclinical study led to unprecedented results in mouse models
Pancreatic cancer is one of the deadliest types of cancer—in the U.S., it is estimated that over 88 percent of people will die from the disease within five years of their diagnosis. One reason for this bleak prognosis is that the majority of pancreatic cancers are diagnosed after the disease has already spread, or metastasized, to other parts of the body. Another reason is that pancreatic cancers are particularly challenging to treat, as these tumors are often resistant to standard anti-cancer drugs.
NIBIB-funded researchers are developing a new method to treat this lethal disease. Their study, recently published in Nature Biomedical Engineering, combined an injectable radioactive gel with systemic chemotherapy in multiple mouse models of pancreatic cancer. The treatment resulted in tumor regression in all their evaluated models, an unprecedented result for this genetically diverse and aggressive type of cancer.
“Radiation treatments are typically delivered externally, which exposes healthy tissue to radiation and limits the dose that a tumor receives, ultimately limiting its effectiveness,” said David Rampulla, Ph.D., director of the division of Discovery Science & Technology at NIBIB. “The radioactive biomaterial investigated in this preclinical study can be injected directly into the tumor, allowing for a localized approach. What’s more, this biodegradable biomaterial allows for higher cumulative radiation doses than other implantable radiation treatments.”
Brachytherapy—where a radiation source is placed inside the body—can be used to treat several different types of cancer. Early-stage prostate cancer, for example, can be treated with ‘seed’ brachytherapy, where many tiny metal seeds that contain a radioactive substance are implanted into the prostate. While these seeds can limit healthy tissues’ exposure to radiation, their metal casing prevents the use of potent radiation particles, known as alpha and beta emitters, which are more effective at killing cancer cells. Additionally, due to their small size, around 100 seeds are typically needed for prostate cancer treatment (with each individual seed requiring an injection). To date, brachytherapy approaches have not improved clinical outcomes among patients with pancreatic cancer.
The current study is investigating a new type of brachytherapy. Instead of delivering radiation using a metal seed or a catheter, the study authors are investigating the use of a radioactive biopolymer that is injected directly into the tumor. In addition to being biodegradable, the biopolymer has a unique property—it has been engineered to transition from a liquid at room temperature to a gel-like state when warmed to body temperature. As the biopolymer solidifies, it stays within the tumor, and can’t easily spread into surrounding healthy tissues.
“Our biopolymer is derived from elastin, an abundant protein that it is found in the connective tissues throughout our bodies,” explained first author Jeff Schaal, Ph.D., who conducted this work at Duke University. “By tinkering with the composition of this biopolymer, we can control the exact temperature where it transitions from a liquid to a gel. And because we’re not encasing the radioactive polymer within a protective metal seed, we can use different—and more potent—isotopes, allowing us to deliver a higher radiation dose than conventional seed brachytherapy.”
The radioactive isotope used in this proof-of-concept treatment is iodine-131 (or I-131), which releases high-energy particles known as beta particles. Beta particles cause DNA damage and kill irradiated cells, but they can’t travel very far—only a few millimeters (so off-target toxicity is limited). I-131 has been used to treat thyroid cancer for decades and has a well-established safety profile, said Schaal.
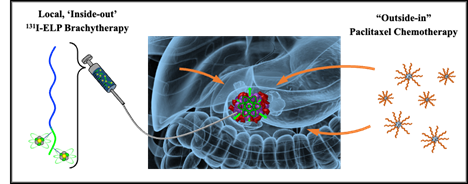
Pancreatic cancer is sometimes treated with a combination of radiation and specific chemotherapeutic agents that make the radiation more effective. These ‘radiosensitizing’ drugs work by prolonging the cell’s replication process—specifically when its DNA is exposed, Schaal explained. The exposed DNA is more sensitive to radiation and is more likely to be irreparably damaged by it, which ultimately results in cell death.
In combination with a radiosensitizing chemotherapeutic known as paclitaxel, the study authors evaluated their radioactive biopolymer in several different pancreatic cancer models, carefully selected to reflect different aspects of pancreatic cancer (e.g., common mutations, tumor characteristics, tumor density, or treatment resistance). Among all the models tested, nearly every mouse responded, meaning the tumors either shrunk or completely vanished. “The response rates that we saw in our models were unprecedented,” said Schaal. “After a thorough review of the literature, we have yet to find another treatment regimen that demonstrates such a robust response in multiple and genetically diverse models of pancreatic cancer.” Further, in some mice, the tumors never returned during the course of the study.
When the study authors evaluated a current clinical treatment regimen—paclitaxel plus external beam radiation—the response rates weren’t nearly as impressive: Tumor growth rate was only inhibited, instead of tumors shrinking or vanishing. “Unlike external beam radiation, which is given in short bursts, our brachytherapy approach delivers radiation continuously,” explained Schaal. “We found that this continuous beta-particle radiation altered the microenvironment of the tumor and allowed paclitaxel to better penetrate into the tumor core, allowing for a synergistic therapeutic effect.”
Importantly, the researchers did not observe any acute toxicity issues during the course of their study, with negligible amounts of radioactivity accumulating in critical organs in the mice. They have previously reported that their radioactive biopolymer safely biodegrades—with the half-life of the gel (roughly 95 days) far outlasting the half-life of I-131 (roughly eight days).
The authors did not evaluate their treatment in metastatic disease, but the nature of their approach would allow for biopolymer injections in multiple locations, such as tumor masses in other organs. And while this study remains in the preclinical stage, the study authors are working to move this treatment forward. “Our group has been partnering with clinical researchers to develop and optimize our system for endoscope-guided delivery in a larger animal model,” said senior author Ashutosh Chilkoti, Ph.D., a professor in the Department of Biomedical Engineering at Duke University. “The challenge however of taking this—or any new treatment—to patients is finding the support to take it through clinical trials.”
This study was supported by a grant from NIBIB (R01EB000188) and a grant from the National Cancer Institute (NCI; grant R35CA197616).
This Science Highlight describes a basic research finding. Basic research increases our understanding of human behavior and biology, which is foundational to advancing new and better ways to prevent, diagnose, and treat disease. Science is an unpredictable and incremental process—each research advance builds on past discoveries, often in unexpected ways. Most clinical advances would not be possible without the knowledge of fundamental basic research.
