Scientists aim to eavesdrop on brain-stomach chemical conversations
Research into what is known as the gut-brain axis continues to reveal how the brain and gut influence each other’s health and well-being. Now researchers are endeavoring to learn more about gut-brain discourse using a model system built in a lab dish.
It has been known for decades that the brain and the gut, which includes the stomach and intestines, have a relationship that relies on open lines of communication. Scientific studies have demonstrated that gut-brain signaling controls basic functions—like a full stomach signaling the brain to stop eating — and has become implicated in the development of complex conditions including depression and auto-immune disease.
And then there are our own conscious experiences that include “trusting our gut,” when faced with a tough decision, getting queasy watching the shower scene in Psycho, or feeling butterflies when that certain someone walks into the room.
Now researchers at the University of Maryland at College Park have engineered an experimental gut-brain system in a lab dish—often referred to as a lab-on-a-chip—to begin to identify the molecules and signaling pathways by which these separate yet interdependent organ systems communicate.
“This is impressive tissue, chemical and electrical engineering,” explained David Rampulla, Ph.D., director of the program in Synthetic Biology at the National Institute of Biomedical Imaging and Bioengineering (NIBIB). “The team designed a chip that could support multiple tissue types while integrating chemical and electrical sensors able to reliably pick-up the subtle signaling taking place between the tissues in real time.”
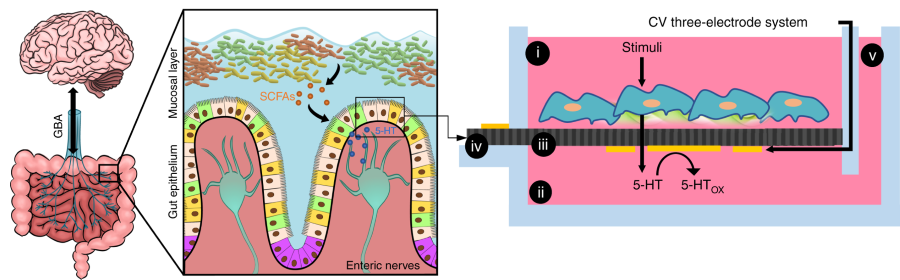
The final chip design features what the team describes as a transwell system. It has a separate compartment for the “mini-gut” made up of endothelial cells that constitute the model of the gut lining, and a separate compartment for the “mini-brain,” a model nervous system made up of the abdominal nerve cord dissected from a crayfish. The crayfish nerve was used because the crayfish has been a staple animal model for the study of gut-brain axis signaling. A fluid connection between the two compartments allowed for movement and monitoring of signaling molecules.
Having designed and built their gut-brain model, the research team performed initial tests. One of the central signaling molecules known to play a key role in gut-brain signaling is the neurotransmitter serotonin. The team injected serotonin into the top of the gut module. The sensors in the system indicated that the neurotransmitter was successfully transferred through the endothelial cell surface through to the base of the endothelium where serotonin is naturally released in the gut.
Within milliseconds, electrical sensors detected firing of neurons in the crayfish nerve indicating that the serotonin had rapidly diffused into the nerve module—faithfully reproducing the natural electrophysiological responses observed in animal studies using the crayfish model.
The team is confident that their system will allow real-time monitoring of signaling between both gut-brain axis tissues simultaneously for the first time without the need to perform invasive procedures on humans or animals.
Future studies planned for the system include examining how electrical signals from the crayfish nerve cord cause changes in endothelial cells that are associated with endothelial dysfunction resulting in disease. For example, in auto-immune diseases such as irritable bowel syndrome, there is a thinning of the gut endothelium that results in endothelial dysfunction and inflammation. Studies in the new system could be extremely valuable for identifying neurochemical signaling involved in disease development and guide new treatment approaches for such complex diseases.
The work was reported in the journal Microsystems & Nanoengineering1 and supported through grants from the National Science Foundation, the National Institute of Biomedical Imaging and Bioengineering, and the University of Maryland’s Brain and Behavior Initiative (BBI) Seed Grant Program.
2. Open Access: http://creativecommons.org/licenses/by/4.0/.
