First Place
TB or Not TB: A First of its Kind Smart Pill to Fill the Pediatric Gap, Purdue University
Jordan Addison, Amelia Adelsperger, Amy Koester, Daniel Romano, Julia Swartzenberg

The pill collects a gastric acid sample from pediatric patients who cannot cough hard enough to provide a sputum sample. If diagnosed early, and with the correct antibiotic treatment, 93% of patients with TB survive. However, diagnosis is difficult for pediatric patients who lack the force to cough up sputum, and instead swallow it. Current diagnostic practices are invasive, require stable electricity, and must be overseen by a trained clinician. In low resource settings it can be difficult, if not impossible, to conduct these procedures. The smart pill is swallowed and collects gastric samples from the stomach. It stays intact as it moves through the digestive system. The sample, which contains traces of the swallowed sputum, is then analyzed for TB. The pill is low-cost, far less painful for the children, and can be used in areas where experts are not available.

Second Place
Point-of-Care Sepsis Stratification, University of Illinois at Urbana-Champaign
Emilee Flaugher, Manish Patel, Michael Rappleye, Ishan Taneja, Sam Wachspress, Jake Winter
The team developed a disposable chip that detects biomarkers of sepsis, a potentially life-threatening response to infection, with higher sensitivity and specificity than is currently possible. Sepsis is diagnosed in up to 1.5 million people in the United States annually, more than breast cancer, prostate cancer, and HIV/AIDS combined. Because survival rates drop with each passing hour after onset of sepsis, this specific and sensitive early detection device could become an important life saving tool.
Click here to watch a video on this project
Third Place (Tie)
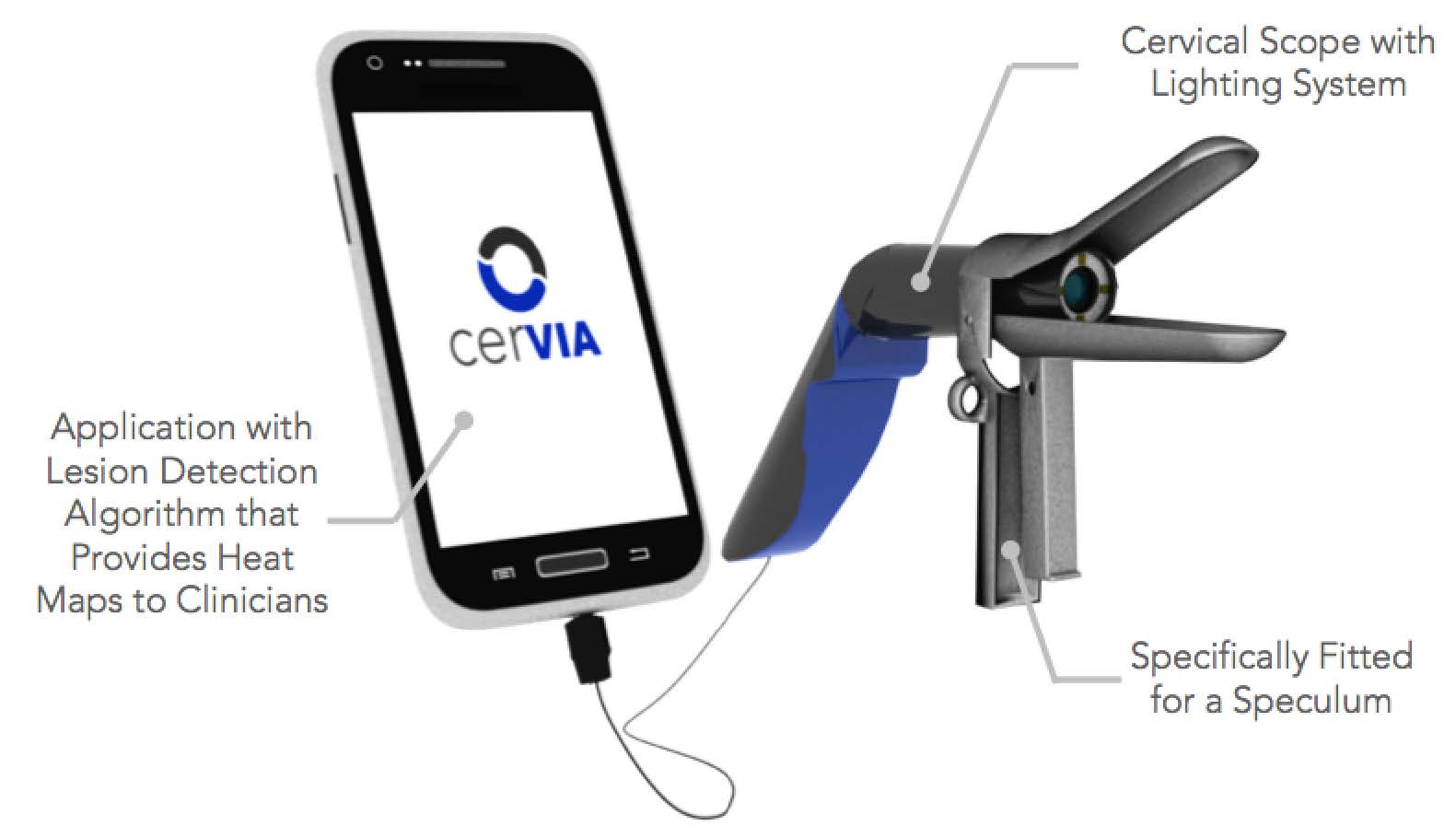
cerVIA, Columbia University
Jahrane Dale, Olachi Oleru, Ritish Patnaik, Stephanie Yang
The cerVia integrates a speculum-fitted custom camera system with cancer detection algorithms to create a handheld cervical cancer detection device that can be used with a smartphone. The cerVIA system seamlessly integrates into the VIA workflow and fits within standard speculums. The custom camera system contains a LED ring and diffusion filters to standardize input images for precancerous lesion detection, consistently capturing images with similar brightness, hue and saturation values. The algorithm then outputs heatmaps to highlight problem areas that clinicians can use to make more-informed diagnoses.
Click here to watch a video on this project
CatheCare, Columbia University
Aonnicha Burapachaisri, Charles Pan, Aishwarya Raja, Chanond Sophonpanich
Central venous catheters (CVCs) are used for many functions like delivering drugs or fluids and drawing blood. They are relatively long-term and remain in place for 3 months or longer. As a result, they are highly susceptible to bacterial colonization that eventually leads to biofilm formation. The CatheCare was created to address the shortcomings of current preventative strategies against bacterial contamination. It is an easy-to-use, non-obstructive, safe, and effective device that eradicates 99.9% of bacteria using germicidal ultraviolet-C light. It also helps prevent biofilm formation on the catheter and reduce the mortality rate and costs associated with catheter-related bloodstream infections.
Click here to watch a video on this project
Venture Prize
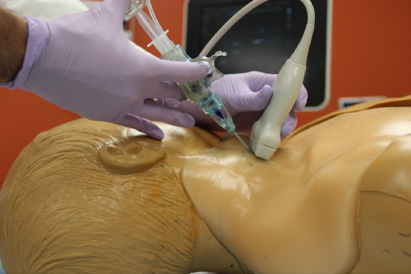
Ballistra Guidewire Advancer, Yale University
Jonathan Dorsch, Brandon Hudik, Andres Ornelas-Vargas
This device was designed to help physicians place a central venous catheter, or central line, in patients. Placing a central line in a patient is not an easy procedure and mistakes are made up to 10% of the time, risking injury to nearby tissues and arteries. The Ballistra Guidewire Advancer was designed to allow physicians to place a central line with one hand instead of two, which means they can simultaneously use an ultrasound device to guide the placement of the needle in the vein. This could greatly reduce the number of errors made during the procedure.
Click here to watch a video on this project
Design Excellence Prize
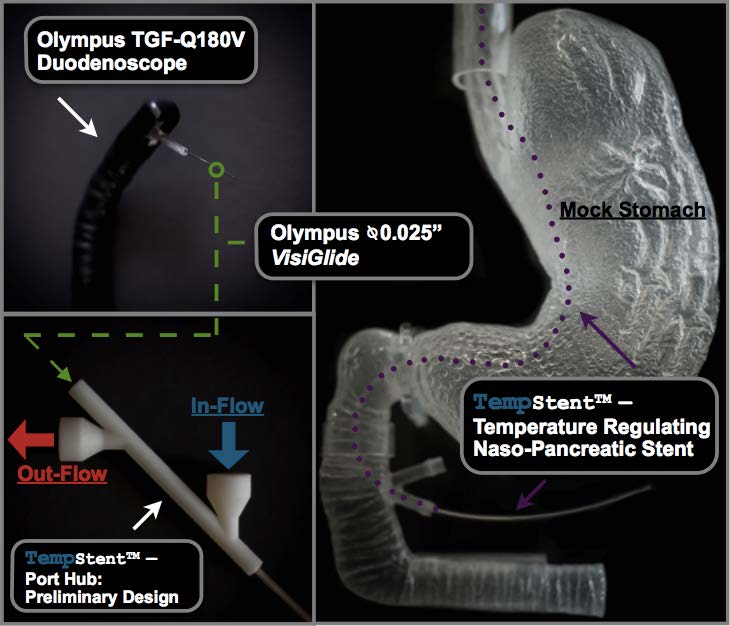 The TempStentTM, Temple University
The TempStentTM, Temple University
Click here to watch a video on this project
Honorable Mentions
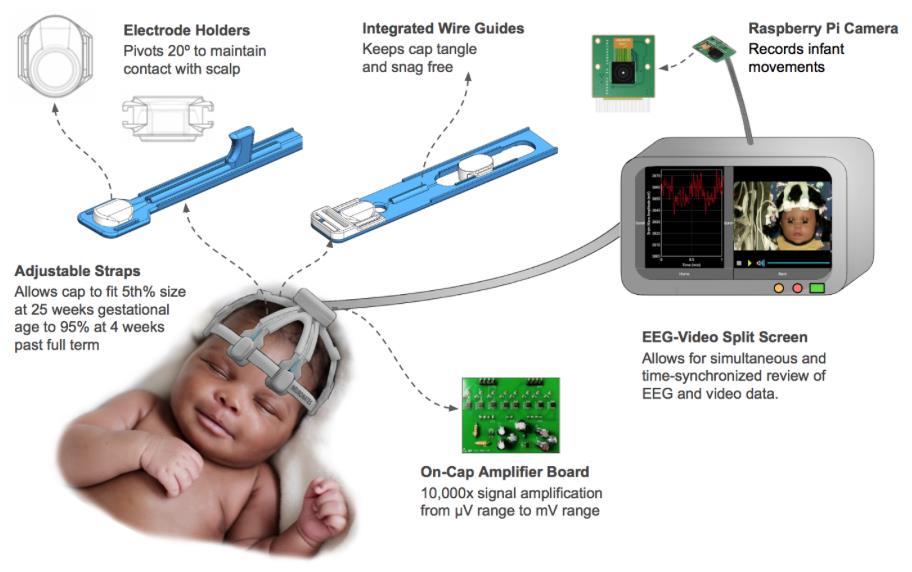
BabyWaves Monitor, Rice University
James Allred, Grant Belton, Leo Meister, Yusi Ou, Momona Yamagami
The device is a low cost, intuitive, reusable, and complete neonatal EEG monitor to address the lack of proper neurological care in low and middle income countries in Sub-Saharan Africa. The system implements a combination of brain activity and video monitoring in order to increase the accuracy and efficacy of seizure diagnoses. It is battery powered, requires no consumables, and maintains individual patient data storage for easy access.
Click here to watch a video on this project

Tendon Reinforcement for Rotator Cuff Repair, Drexel University
Michael Chen, Desiree Martini, David Rodak, Kenneth Rodriguez
To reinforce rotator cuff repairs and limit the chance of a re-tear, this novel tendon reinforcement device was developed to strengthen suture-tendon interfaces. This device is implantable into tendons and provides a protective barrier between sutures and tendon and results in a more even distribution of suture tension experienced by tendon.
Click here to watch a video on this project
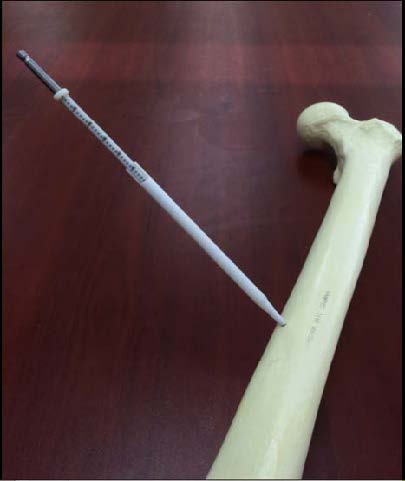
The Sleeve: A Novel Bone Screw Depth Gauge, Clemson University
Justin Bacaoat, Alison Farrell, Katherine Hafner, Mariah McMinn, Harrison Smallwood
A novel method of determining the depth drilled into bone that is more efficient than existing depth gauges and more accommodating for larger patients. It addresses the issue of improperly measured screws while also increasing efficiency in surgery by reducing
the number of steps in the measuring process.
Click here to watch a video on this project

Gel-Aid, Stanford University
Shivani Baisiwala, Celina Malave, Christopher Mathy, Kaelo Moahi
The Gel-Aid was desgined to improve on the standard of care for the wound care of surgical patients. The Gel-Aid--an absorbable, removable, alginate-based hydrogel--is capable of absorbing exudate over 100 times its dry weight in 24 hours while still keeping wounds moist. This swelling ratio is more than enough to capture the pus in these types of wounds. It needs to be changed only once per day and requires minimal interaction from the patient.

