- What are image-guided robotic interventions?
- What are the advantages of minimally invasive procedures?
- What are some examples of image-guided robotic interventions and how are they used?
- What are NIBIB-funded researchers developing in the area of image-guided robotic interventions to improve medical care?
What are image-guided robotic interventions?
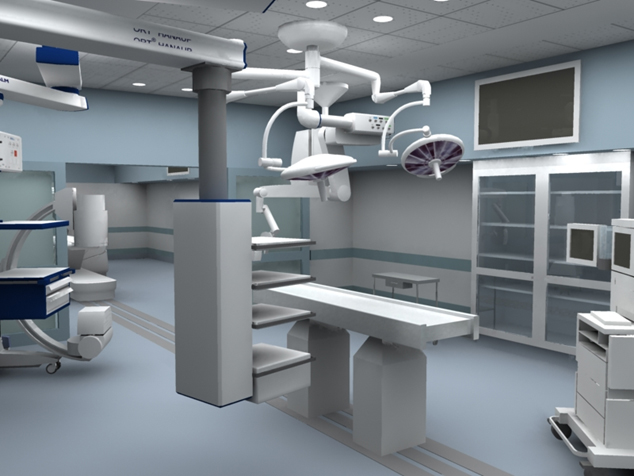
Image-guided robotic interventions are medical procedures that integrate sophisticated robotic and imaging technologies, primarily to perform minimally invasive surgery. This integrated technology approach offers distinct advantages for both patients and physicians.
Imaging: In image-guided procedures, the surgeon is guided by images from various techniques, including magnetic resonance (MR) and ultrasound. Images can also be obtained using tiny cameras attached to probes that are small enough to fit into a minimal incision. The camera allows the surgery to be performed using a much smaller incision than in traditional surgery.
Robotics: The surgeon’s hands and traditional surgical tools are too large for small incisions. Instead, thin, finger-like robotic tools are used to perform the surgery. As the surgeon watches the image on the screen, she uses a tele-manipulator to transmit and direct hand and finger movements to a robot, which can be controlled by hydraulic, electronic, or mechanical means.
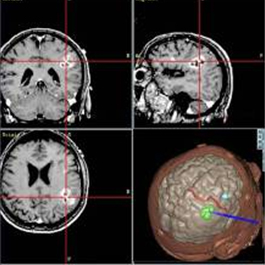
Robotic tools can also be controlled by computer. One advantage of a computerized system is that a surgeon could potentially perform the surgery from anywhere in the world. This type of long distance surgery is currently in the experimental phase. The experiments illustrate the life-saving potential for such surgeries when a delicate operation requires a specially trained surgeon who is in a distant location.
Additionally, doctors can use image-guided robotic interventions to more accurately target tumors when performing biopsies and radiation treatments.
What are the advantages of minimally invasive procedures?
Minimally invasive surgery can reduce the damage to surrounding healthy tissues, thus decreasing the need for pain medication and reducing patients’ recovery time. For surgeons, image-guided interventions using robots also have the advantage of reducing fatigue during long operations, allowing the surgeon to perform the procedure while seated.
What are some examples of image-guided robotic interventions and how are they used?

Robotic prostatectomy: Complete prostate removal is performed through a series of small incisions, compared with a single large incision of 4 to 5 inches in traditional surgery. The small incisions result in a shorter post-operative recovery, less scarring, and a faster return to normal activities.
Ablation techniques for early cancers: Patients with early kidney cancer can be treated with minimally invasive procedures to destroy small tumors. Cryoablation uses cold energy to destroy the tumors. Doctors use computed tomography (CT) and ultrasound imaging to position a needle-like probe within each kidney tumor. Once in position, the tip of the probe is super-cooled to encase the tumor in a ball of ice. Alternate freeze/thaw cycles kill the tumor cells. Other minimally invasive methods of destroying early kidney cancers include heating the tumor cells, and surgical removal using a robotic device. Many patients can go home the same day and are able to perform regular activities in several days.
Orthopedics: Image-guided robotic procedures are improving the precision and outcome of a number of orthopedic procedures. For example, partial knee resurfacing surgeries aim to target only the damaged sections of the knee joint. Orthopedic surgeons are combining the use of a robotic surgical arm and fiber optic cameras in such procedures, which results in patients retaining more of their normal healthy tissue. Image-guided robotic procedures also improve total knee replacements, allowing precise alignment and positioning of knee implants. The result is more natural knee function, better range of motion, and improved balance for patients.
What are NIBIB-funded researchers developing in the area of image-guided robotic interventions to improve medical care?
 Portable robot uses 3D near-infrared imaging to guide needle insertion into veins:
Portable robot uses 3D near-infrared imaging to guide needle insertion into veins:
Drawing blood and inserting IV lines are the most commonly performed medical procedures in hospitals and clinics. However, for many patients it can be difficult to find veins and accurately insert the needle, resulting in patient injury. NIBIB-funded scientists are developing a portable, lightweight medical robot to help perform these procedures. The device uses 3D near- infrared imaging to identify an appropriate vein for the robot to insert the needle. The current goal is to integrate the imaging system and software into a miniaturized version of the prototype robot. The outcome will be a compact, low-cost system that will greatly improve the safety and accuracy of accessing veins.
Robot-assisted needle guidance aids removal of liver tumors:
Radiofrequency ablation (RFA) is a minimally invasive treatment that kills tumors with heat and can be a life-saving option for patients who are not eligible for surgery. However, broad use of RFA has been limited because the straight paths taken by the needles that carry tumor-killing electrodes may damage lung or other sensitive organs. Also, large tumors require multiple needle insertions, which increases bleeding risk. To address the problem of tissue damage using straight needles, NIBIB-funded scientists are developing highly flexible needles that can be guided along controlled, curved paths through tissue, allowing the removal of tumors that are not accessible by a straight-line path. The technology combines needle flexibility with a 3D ultrasound guidance system that allows the doctor to correct the path of the needle to avoid unexpected obstacles as the needle advances toward the tumor. The device will ultimately increase the accuracy and reduce the damage to healthy tissue during tumor removal resulting in wider use of the technology for better patient outcomes.
Swallowable capsule identifies and biopsies abnormal tissue in the esophagus:
Barrett’s esophagus is a precancerous condition that requires repeated biopsies to monitor abnormal tissue. NIBIB-funded researchers are developing a swallowable, pill-sized device to improve the management and treatment of this condition. The unsedated patient can easily swallow the pill, which is attached to a thin tether made of cable and optic fiber. The device detects microscopic areas of the esophagus that may show evidence of disease, and uses a laser to collect samples from the suspicious tissue—a technology known as laser capture microdissection. The physician then retrieves the device from the patient without discomfort and the collected micro-samples are examined for visual evidence of disease, as well as genetic analysis. This minimally invasive device improves patient comfort and provides a precise molecular profile of the biopsied regions, which helps the physician to better monitor and treat the disorder.
Reviewed July 2016
